Drug calculations for all healthcare professionals
Commonly used abbreviations
NOTE: Many Trusts’ drug policies state that certain abbreviations should not be used in prescriptions because they are a source of errors if misunderstood.
Usually accepted abbreviations
Kilogram= kg
gram= g
Milligram= mg
Microgram= should always be written as microgram
Nanogram= should always be written as nanogram
liter= L
millilitre= ml or mL
units or international units= should always written as units or international units
millimoles= mMol or mmol
Note
The use of fractional doses is unsafe and should be avoided
Example
0.1g should be written as 100mg
0.5mg should be written as 500 micrograms
The unnecessary use of decimal points should be avoided e.g. 3mg, not 3.0mg.
Converting units of weight and volume
Metric units of measurement to Weight
1kg = 1000g
1g = 1000mg
1mg = 1000 micrograms
1 microgram = 1000 nanograms
Volume
1L =1000ml
1ml Weighs 1g
1000ml Weighs 1000g or 1kg
10- or 100-fold errors can occur if dosing units are converted incorrectly.
Principles
Doses may be calculated by body weight or body surface area.
Example 1
A prescription for metformin 1g. How many milligrams is this?
To convert grams to milligrams multiply by 1000 1g = 1 x 1000 = 1000mg
Example 2
A patient is prescribed 0.0625mg digoxin. How many micrograms is this?
To convert milligrams to micrograms multiply by 1000 0.0625mg = 0.0625 x 1000 micrograms = 62.5 micrograms
Example 3
Amiodarone 5mg per kg body weight in 100ml 5% glucose over 20 mins is prescribed. The patient weighs 60kg.
To calculate the dose
Dose = 5(mg) x 60(kg) = 300mg
Calculating concentrations
Principles
The way the strength of a drug in a solution is described will affect the way a dose calculation is carried out. Doses may be expressed in a number of different ways:
- Mass (weight) per volume of solution, e.g. mg in 10ml, mMol/L.
- Units of activity per volume of solution, e.g. units per ml.
- Percentage. This is the weight of the drug in grams that is contained in each 100ml of the solution. Common examples are 0.9% sodium chloride; 5% glucose.
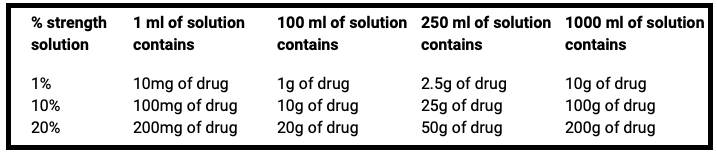

Note
- If you know the number of grams in 1000ml, divide by 10 to convert to % strength
• If you know the % strength, multiply by 10 to give the number of grams of drug in 1000ml
• If you know the % strength, divide by 100 to calculate the amount of drug in 1ml
Example 1
The prescribed dose is 1g magnesium sulphate. Magnesium sulphate 50% injection is available. 50% = 50g in 100ml.
How many ml contains 1g magnesium sulphate?
Number of ml containing 1g = (100ml x1g)/50g = 2ml
Another way of thinking about this is: 50g in 100ml = 5g in 10ml = 1g in 2ml
Example 2
Thiopentone 2.5% infusion is prescribed. What volume is required to administer a dose of 100mg? 2.5% = 2.5g in 100ml
100mg is contained in (100mg x 100ml)/2500mg = 4ml
Another way of thinking about this is:
Thiopentone 2.5% = 2.5g in 100ml = 2500mg in 100ml = 25mg in 1ml = 100mg in 4ml
Ratios
The strengths of some drugs such as adrenaline (epinephrine) are commonly expressed in ratios.

1 in 1000 solution of adrenaline contains 1g in 1000ml = 1000mg in 1000ml = 1mg in 1ml
1 in 10,000 solution of adrenaline contains 1g in 10,000ml = 1000mg in 10,000ml = 1mg in 10ml
Ratios
Example 1
Adrenaline (epinephrine) 1 in 1000 injection is available. The prescribed dose is 1ml.
How many mg in 1ml?
Use a two-step process:
The solution contains 1g in 1000ml
Step 1: 1g in 1000ml = 1g/1000ml in 1ml
Step 2: Convert this to mg by multiplying by 1000
(1g x1000)/1000ml = 1mg in 1ml
Another way of thinking about this is: 1g in 1000ml = 1000mg in 1000ml = 1mg in 1ml
Calculating oral doses in tablets
Principles
- Check the strength of (amount of drug in) each tablet or capsule.
- Make sure you are clear about the dose units used, most commonly prescribed are milligrams
or micrograms. - Check the dose on the prescription and that it is expressed in the same units as on the medicine label.
- If the prescription and the medicines label use different units of strength, refer to the conversion table and calculation examples.
- Once you are sure that the units are the same, divide the required dose by the strength of the tablet or capsule.
- The answer is the number of tablets/capsules needed for each dose.
Number of tablets = Dose/Strength of tablet
Extra safety tip
If your first calculation gives a dose of more than two tablets, double-check the calculation and confirm that the dose doesn’t exceed the manufacturer’s recommended maximum. If it does, or if you are still unsure that the dose is correct, check with the prescriber or pharmacist.
Calculating oral doses in tablets
Example 1
Amoxicillin 500mg three times a day p.o. is prescribed. Amoxicillin capsules 250mg are available.
The number of capsules needed for each dose = 500mg/ 250mg = 2 capsules
Example 2
Levomepromazine 6.25mg three times a day p.o. is prescribed. Levomepromazine tablets 25mg are available.
The number of tablets needed for each dose = 6.25mg/ 25mg = 0.25 or 1⁄4 of a tablet
Another way of looking at this is:
Half a tablet = 25mg/ 2 = 12.5mg
Quarter of a tablet = 25mg/ 4 = 6.25mg
Calculating oral doses for children and neonates
Principles
- Always use the smallest oral syringe that will hold the volume you need to measure.
- If the dose prescribed means that less than a whole tablet or capsule is required, check with
the pharmacy that it is appropriate to break a tablet or split a capsule before doing so. - If it is essential, dissolve or disperse the powder/crushed tablet in an accurately measured amount of water (e.g. 5ml). Stir and draw up the required volume immediately.
Volume required = (Dose in mg x Volume of solution)/ Amount of drug (mg) in tablet - If the result cannot be accurately measured, e.g. 0.33ml, it is generally acceptable to round the dose up or down. However, the actual dose given must be within 10% of the calculated dose. If this cannot be achieved, discuss it with the prescriber and pharmacist.
Example 1
2mg amlodipine p.o. is prescribed. 5mg amlodipine tablets are available. Crush one tablet and mix the powder thoroughly in 5ml of water.
The dose required is: (2mg x 5ml)/ 5mg = 2ml
Another way of thinking about this is: 5mg in 5ml = 1mg in 1ml = 2mg in 2ml
Example 2
14mg ranitidine p.o. is prescribed.
15mg per ml ranitidine oral suspension is available.
The dose required is: (14mgx 1)/ 15mg = 0.933ml
0.933ml cannot be accurately measured but 0.9ml or 1ml could be. 1ml is the easiest to measure, which equates to 15mg ranitidine. To work out the % increase: (15mg x 100)/ 14mg = 107%
A 7% increase is less than 10% above the prescribed dose of 14mg so is acceptable. 15mg (1 ml) can be accurately measured and should be given.
Calculating IV drug doses
Principles
- For drugs already in solution, check the amount of drug in each ml and the total amount of drug in the container.
- Make sure you are clear about the dose units used. Most commonly prescribed are milligrams (mg) or micrograms.
- Beware of drugs such as insulin and heparin, for which doses are prescribed in international units (which is sometimes, but should never be, abbreviated to i.u. which can be misread as 10).
- Check the dose on the prescription and that it is expressed in the same units as on the medicine label.
- If the prescription and the medicines label use different units of strength, refer to the conversion table and calculation examples on pages 4 and 5.
- Once you are sure that the units are the same, divide the required dose by the amount of the drug in the ampoule and multiply by the volume of solution in the vial or ampoule.
- The answer is the volume needed for each dose.
Volume required = (Dose x Volume of solution in ampoule)/ Amount of drug in ampoule
Example 1
Digoxin 125 microgram in 100ml sodium chloride 0.9% is prescribed over 1 hour. 500 microgram digoxin in 2ml ampoules are available.
The volume to be added to 100ml sodium chloride 0.9% is:
(125 micrograms x 2ml)/ 500 micrograms = 0.5ml
Example 2
300mg aminophylline injection is prescribed. 250mg in 10ml ampoules are available. The volume of injection required is:
(300mg x 10ml)/ 250mg = 12ml
Calculating drip rates for gravity flow infusions
Principles
- Without a flow control device such as a pump, infusion rates depend entirely on gravity. The rate of flow is measured by counting drops per minute.
- Administration sets deliver controlled amounts of fluid at a predetermined fixed rate, measured in drops per minute.
- It is also important to check the number of drops per ml delivered by the administration set (which is printed on the outer packaging). This may vary between sets, between manufacturers and between different infusion fluids or drug solutions.
- A (drug) solution administration set will usually deliver 20 drops per ml of clear infusion fluid such as 0.9% sodium chloride injection.
- A blood administration set will deliver 15 drops per ml of blood.
- A burette administration set will usually deliver 60 drops per ml of infusion fluid or drug solution.
- Number of drops per minute = (Volume in ml x Number of drops per ml)/ Intended duration of infusion (in minutes)
Example 1
1000ml sodium chloride 0.9% infusion over 8 hours using a solution set is prescribed. 8hr = 8 x 60min. The drip rate needs to be set at:
(1000ml x 20 drops per ml)/ 8 x 60min = 20000 drops/ 480min = 42 drops per minute
Example 2
1 unit of blood over 4 hours using a blood set is prescribed. (1 unit of blood = 350ml.) 4hr = 4 x 60min. The drip rate per minute should be set at:
(350ml x 15 drops per ml)/ 4 x 60min = 5250 drops/ 240min = 22 drops per minute
Example 3
100ml glucose 5% infusion over 6 hours using a burette set is prescribed. 6hr = 6 x 60min. The rate per minute should be set at:
(100ml x 60 drops per ml)/ 6 x 60min = 6000 drops/ 360min = 17 drops per minute
Calculating infusion rates for infusion devices
Principles
- Also, see the principles on page 18.
- All infusions require rate control. This can be achieved using a roller clamp (gravity flow),
an infusion pump, a syringe driver, a syringe pump or a disposable device. - When using any sort of rate control device, check at least the following parameters at regular intervals in accordance with local policy:
• Volume given
• Volume remaining
• Administration rate
• Condition of the patient including the administration site - Before and after the transfer of care between units or teams, make sure you repeat the above checks.
- You should always check the manufacturer’s instructions or refer to local policy to ensure you use the correct administration set for the device and that the device is programmed correctly.
- An administration device should only be used by practitioners who have been trained and are competent in the use of the particular device.
The rate may be prescribed in terms of:
Volume: For example ml per hour or ml per min. OR:
Amount of drug: For example mg per min or international units per hour.
Volume in ml per hour: Total volume of infusion (ml)/ Duration of infusion (hour) = ml per hour
Amount of drug in mg per hour: Total dose in mg/ Duration of infusion (hour) = mg per hour
Example 1
To calculate the amount of infusion to be given in ml per hour.
500ml sodium chloride 0.9% is prescribed to be given over 4 hours using a volumetric pump.
The rate of infusion should be set at:
500ml/ 4 hour = 125ml per hour
Example 2
Diamorphine 30mg in 60ml 0.9% sodium chloride over 24 hours using a syringe pump is prescribed. To be given at 1.25mg per hour. How many ml per hour should be given?
The number of mls containing 1mg = Volume of infusion (ml)/ Amount of drug (mg) = 60ml/ 30mg = 2ml
The number of mls containing 1.25mg = 2 (ml) x 1.25 (mg) = 2.5ml
Therefore, 2.5ml per hour will deliver 1.25mg per hour.
Example 3
A similar method can also be used to calculate the rate of an insulin infusion.
Insulin 50 international units in 50ml 0.9% sodium chloride is prescribed for administration from a syringe pump, starting at 4 international units per hour.
The rate should be set at: (Volume infusion x Dose of drug per hour)/ Amount of drug
= (50ml x 4 international units per hour)/ 50 international units = 4ml per hour
Another way of thinking about this is:
50 international units in 50ml = 1 international unit in 1ml = 4 international units in 4ml
Calculating rates for syringe drivers
Principles
- A syringe driver pushes the plunger of a syringe forward at an accurately controlled rate.
• For most syringe pumps the rate is set according to the volume of solution injected per hour, i.e. in ml per hour
• For some syringe drivers the rate is set according to the distance traveled by the plunger in mm per hour or mm per 24 hour - If the rate is to be set in mm, the volume to be administered by a syringe driver depends on
the diameter of the syringe barrel as well as on the rate setting. Different makes of syringe may have different barrel sizes. It is essential that the brand of syringe to be used is specified and the stroke length is measured. - Serious errors have occurred when settings in mm per hour and ml per hour have been confused.
- Prepare prescribed infusion
- Prime the extension set with fluid
- If using a syringe driver, measure the stroke length (the distance the plunger has to travel) in mm.
See diagram for example
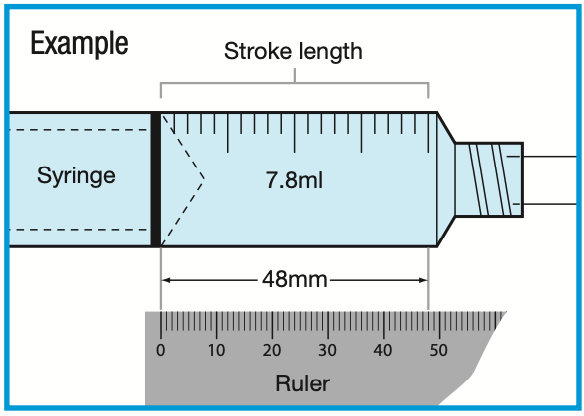
Principles continued
- Check carefully the units of time in which the syringe driver operates: Is the rate set in mm per hour or mm per day (24 hours)?
mm per hour
Rate = Stroke length (mm)/ Infusion period (hours)
mm per 24 hours
Rate = Stroke length (mm)/ Infusion period (days)
Example 1
Diamorphine 20mg over 12 hours is prescribed. The stroke length is measured as 48mm.
The rate-setting needed on a mm per hour syringe driver is: 48mm/ 12 hours = 4mm per hour
Example 2
Diamorphine 20mg over 1 day (24 hours) is prescribed. The stroke length is measured as 48mm.
The rate-setting needed on a mm per 24-hour driver is: 48mm/ 1 day = 48mm per 24-hour
Calculating IV drug doses for children and neonates
Principles
- Remember that many injections are made for adults. For children’s doses, you may need as little as one-tenth (1/10) or even one hundredth (1/100) of the contents of one ampoule or vial.
- When calculating infusions, consider the child’s total daily fluid allowance. More concentrated individual infusions may be required. Discuss with the pharmacist or prescriber.
- Ensure the prescribed infusion fluid/diluent is appropriate for the child e.g. the sodium content of an infusion contributes to the child’s total daily sodium requirement.
- For many injections presented as powders for reconstitution, the powder adds to the volume of the final solution after the diluent has been added. This ‘displacement value’ must be taken into account when the dose needed is less than the full contents of the vial or ampoule.
The displacement value can be found on the package insert. It may vary with brands, so it is crucial to check the package insert for the product you are actually using.
5. For the above reasons, the calculations involved in preparing and administering infusions for children are often particularly complex. It is most important that these calculations are independently checked.
Example 1
A brand of amoxicillin 250mg vials has a displacement value of 0.2ml per vial.
This means that for this brand, 250mg of the powder occupies a volume of 0.2ml.
Therefore, if you add 5ml to the vial, the resulting solution contains 250mg amoxicillin in 5.2ml. To make a solution containing 250mg in 5.0ml, you must add 4.8ml of WFI.
Example 2
How many mmols of Na would a child receive from an infusion of sodium chloride 0.9% given at a rate of 1ml per hour over 24 hours?
0.9% sodium chloride contains 150mmol Na per litre (1000ml) = 150mmol per ml/ 1000ml
Number of mmol per 24 hours = (150mmol/ 1000ml) x 24 hour = 3.6mmol Na in 24 hours
This is normally acceptable for a 6-year-old child, but may not be for a neonate.
Example 3
0.5 microgram per kg per minute midazolam is prescribed for a 1kg baby, to run at 0.1ml per hour. The prescription asked for 7.5mg midazolam in 25ml glucose 5%. Ampoules of midazolam 5mg in 5ml are available.
To prepare the syringe as prescribed:
The volume needed for a dose of 7.5mg = (Dose x Volume in ampoule)/ Amount of drug in ampoule
= (7.5mg x 5ml)/5mg = 7.5ml
To make up 7.5mg to 25ml in a syringe:
Draw up a 7.5ml midazolam injection into a 10ml syringe and transfer to a 25ml syringe.
The volume of glucose required = 25ml – 7.5ml = 17.5ml
Add 17.5ml glucose 5% injection to the 25ml syringe to make a total volume of 25ml.
The syringe now contains 25ml of solution containing 7.5mg midazolam.
